By Anupriyo Chakravarti, Chief Technology & Product Officer at Verisma
January 30, 2026
Healthcare data management is at a crossroads. Labor costs have risen 15 percent year–over–year, regulatory complexity continues to expand, and the pressure to do more with less has never been greater. In my conversations with health system CIOs and technology leaders, one theme emerges consistently: the organizations treating AI governance as a strategic capability, not a compliance checkbox, will define the next era of healthcare operations.
I had the opportunity to test this thesis at CHIME25 – Fall Forum, where I led a focus group titled “Rewriting Healthcare Data Rules: Digital Leaders, Innovators, and Disrupters Unite.” We surveyed attendees before the conference to understand how they’re approaching artificial intelligence, legacy systems, interoperability, and vendor relationships. The findings confirmed what I’ve observed across hundreds of client engagements: most organizations recognize AI’s potential, but few have built the governance foundation to capture it safely.
Here’s what the data revealed – and what it means for healthcare technology strategy.
Key Findings: An Industry in Transition
1. Data Governance Ownership Remains Fragmented
CIO/IT leadership drives data governance in most organizations, with joint committees and compliance/legal playing supporting roles. Fewer than 10 percent reported no clear ownership. The implication: Organizations with dedicated governance structures will move faster on AI adoption.
2. AI Training Data Concerns are Real – but Nuanced
While there’s openness to AI innovation, organizations remain vigilant about third–party data access. Most enforce strict controls over vendor use of data for model training. The strategic insight: Healthcare leaders aren’t anti-AI; they’re anti-opacity. Vendors who provide transparency, auditability, and clear data boundaries will earn trust.
3. Interoperability Remains a Multi–Front Battle
While organizations struggle equally with standards adoption, system integration, and partner data sharing, no single blocker dominates. Most have policies in place, but consistency and enforcement vary widely. What this signals: Point solutions won’t solve interoperability. Organizations need integrated platforms – built with universal connectors in addition to APIs – that address the full data lifecycle, from intake through archive.
4. Legacy Decommissioning is Reactive, not Strategic
Most organizations archive legacy systems to mitigate risk rather than as part of a deliberate data strategy. There’s growing openness to monetizing de-identified data for research, but risk concerns dominate decision-making. The opportunity: Organizations shifting from reactive archiving to strategic data lifecycle management can unlock cost savings and new revenue streams.
5. Global Resource Sentiment is Shifting
Opinions on using global resources for data-related tasks lean toward caution, but a meaningful minority, about 25 percent, is open to increased global partnerships. Looking ahead: As AI handles more routine tasks, the calculus around global delivery models will evolve.
The AI Maturity Gap
We asked respondents which stage of AI/data governance maturity best reflects their organization:
- Level 1: Ad hoc tools, minimal governance, data silos
- Level 2: Emerging AI/machine learning use with basic automation and foundational policies
- Level 3: Standardized platforms, governed data, formalized policies
The majority cluster at Levels 1 and 2. Very few have reached Level 3, and almost none have progressed beyond it to advanced stages where AI augments decision–making across operations.
This maturity gap represents a risk and opportunity. Organizations remaining at Level 1-2 will struggle to capture efficiency gains while managing compliance exposure. Those accelerating to Level 3 and beyond can achieve 40-60 percent productivity improvements in data-intensive workflows while strengthening compliance posture.
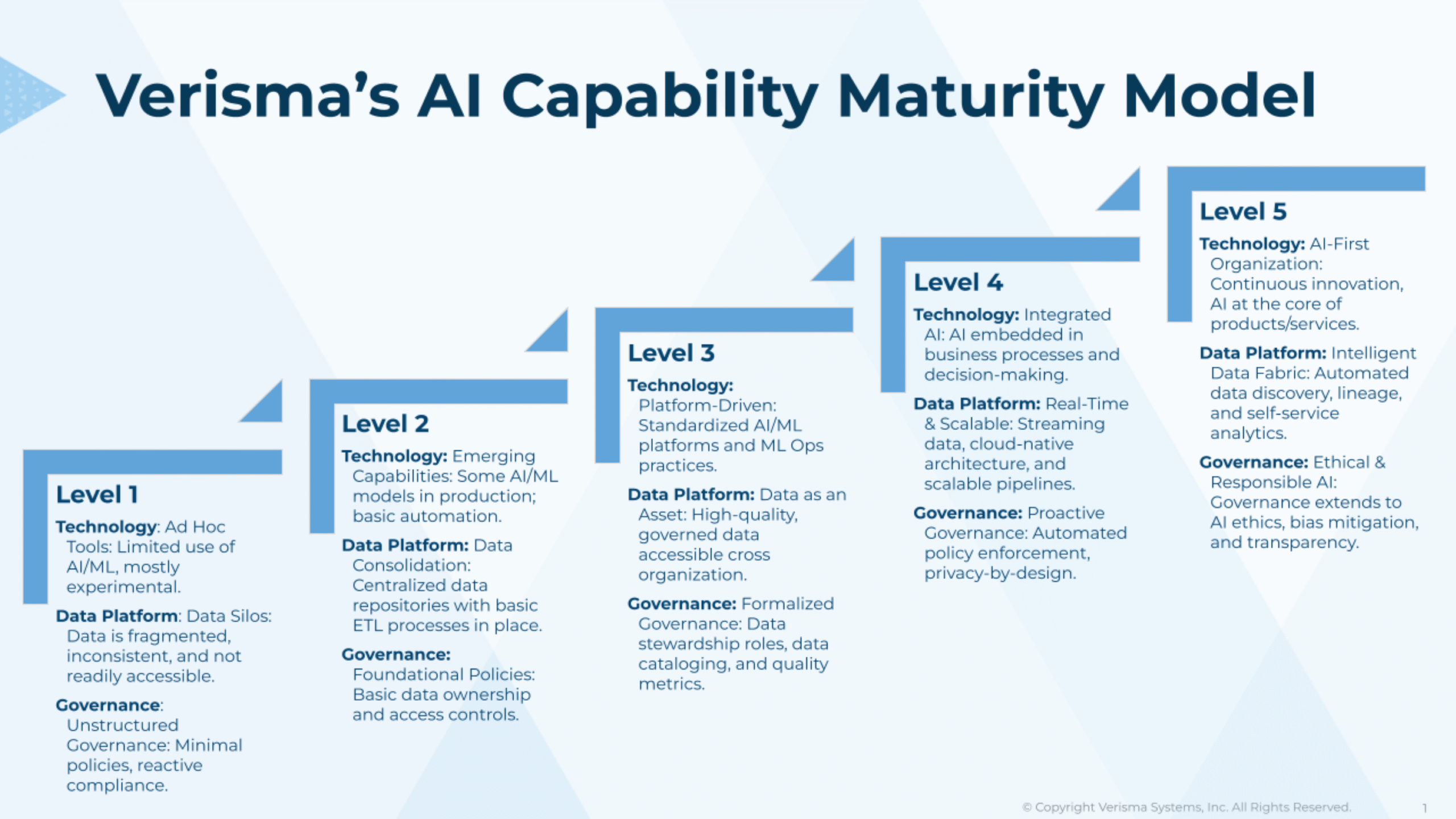
Verisma’s AI Maturity Model: A Framework for Transformation
Based on these findings and our experience partnering with 2,300+ healthcare organizations, we developed an enhanced maturity framework.
The model assesses five dimensions:
1. Technology Infrastructure – From siloed tools to integrated intelligent platforms
2. Data Governance – From ad hoc policies to enterprise–wide standards with automated enforcement
3. Process Automation – From manual workflows to AI–augmented operations
4. Value Realization – From cost–center metrics to measurable business outcomes
5. People and Change – From resistance to adoption to workforce enablement and upskilling
What makes this framework different: It’s not theoretical. Each maturity level includes specific benchmarks, implementation tools, and a phased roadmap with measurable success criteria. We built it for organizations that need to show progress quarterly, not just aspire to transformation over years.
The Strategic Moat: Human-in-the-Loop AI Governance
I’ll share a perspective that may diverge from the industry hype: organizations that win with AI won’t automate the most, they’ll automate responsibly.
Many vendors offer point solutions for robotic process automation or document classification. Verisma’s approach is fundamentally different. We’ve built an integrated platform spanning the full health information lifecycle – intake, retrieval, quality assurance, disclosure, and archiving – with human oversight embedded at every decision point
.
Why does this matter, strategically:
- Regulatory durability: Healthcare AI regulations are tightening. Solutions built on black–box automation face compliance risk. Human-in-the-loop architectures are designed for the regulatory environment that’s coming, not just today’s requirements.
- Quality assurance: Our AI workflows use confidence thresholds automatically triggering human review when certainty falls below acceptable levels. This isn’t a safety net, it’s a design principle. Organizations using this approach achieve 38 percent faster turnaround times while reducing unauthorized disclosure incidents by 50 percent.
- Auditability: Every AI decision is logged with immutable trails, reviewer attestations, and exception documentation. When regulators or auditors ask, “How did this decision get made?” There’s a clear answer.
- Workforce enablement: We don’t replace health information professionals; we amplify them. Staff handle exceptions and complex judgments while AI manages routine processing.
The Path Forward: From Maturity Assessment to Business Outcomes
Based on our CHIME25 research and client experience, here’s what I believe healthcare technology leaders should prioritize:
1. Assess honestly. Most organizations overestimate their AI maturity.
2. Governance before acceleration. The organizations moving fastest on AI adoption aren’t the ones with the biggest budgets. They have the clearest governance frameworks measuring and optimizing outcome metrics.
3. Demand transparency from vendors. Ask tough questions: Where does my data go? How are models trained? What happens when the AI’s uncertain?
4. Measure business outcomes, not AI activity. For instance, for release of information, track turnaround time and compliance incidents, not number of AI models deployed.
5. Plan for workforce transition. AI will change roles, not eliminate them.
Looking Ahead
In the next three years, I expect 75 percent of routine healthcare data tasks to be AI–assisted. The organizations thriving won’t adopt AI first. They’ll build governance, infrastructure, and workforce capabilities to adopt AI well.
Healthcare technology leaders are ready for this transformation. They’re looking for partners understanding operational realities and delivering practical innovation with transparency and accountability. If you’re evaluating your organization’s AI maturity, let’s chat.
About the Author
Anupriyo Chakravarti is Chief Technology & Product Officer at Verisma, leading technology strategy and product development for healthcare’s leading health information management platform. He speaks regularly on AI governance, healthcare data transformation, and technology leadership at industry conferences including AHIMA, CHIME and HIMSS.
