VALUE-BASED CARE ENABLEMENT SOLUTIONS

We power quality initiatives, risk adjustment, and continuation of care workflows,
so providers and plans can focus on what matters most: healthier patients.
BUILT FOR A VALUE-DRIVEN, EVOLVING HEALTHCARE LANDSCAPE
As the shift from volume to value accelerates, medical record demands and retrieval complexities are only growing. Verisma’s deep Health Information Management expertise, earned through 20+ years of Release of Information leadership powers faster, more complete, and fully compliant chart retrievals supporting quality initiatives such as Healthcare Effectiveness Data and Information Set (HEDIS), Merit-Based Incentive Payment System (MIPS), risk adjustment programs (retrospective, prospective and concurrent), and other whole person health needs. Our integrated approach reduces delays and administrative friction, helping you deliver better outcomes with less burden.
Our internal staff work in clearly defined silos when supporting Providers and Payers, ensuring that each party’s data and processes remain fully protected. This intentional separation eliminates overlap, safeguards privacy, and reinforces our commitment to compliance.
SOLUTIONS THAT ADVANCE VALUE-BASED CARE

MEDICAL RECORD RETRIEVAL
Accurate, complete, and timely record collection in every state using the providers’ preferred retrieval method.

ENABLING QUALITY INITIATIVES
Efficient record retrieval following quality measure guidelines to support the chart abstraction process.

ENABLING RISK ADJUSTMENT INITIATIVES
Retrospective, Prospective and Concurrent risk adjustment record retrieval to support coding programs.

REFERRAL MANAGEMENT
Improve member engagement and Star ratings through seamless referral tracking.

PROVIDER ENGAGEMENT
Onsite or remote support to ensure provider collaboration and fast turnaround.

SECOND PASS RETRIEVALS
We recover failed or incomplete retrievals to reduce administrative burden.

TRUSTED BY LEADERS ACROSS HEALTHCARE

20,000+
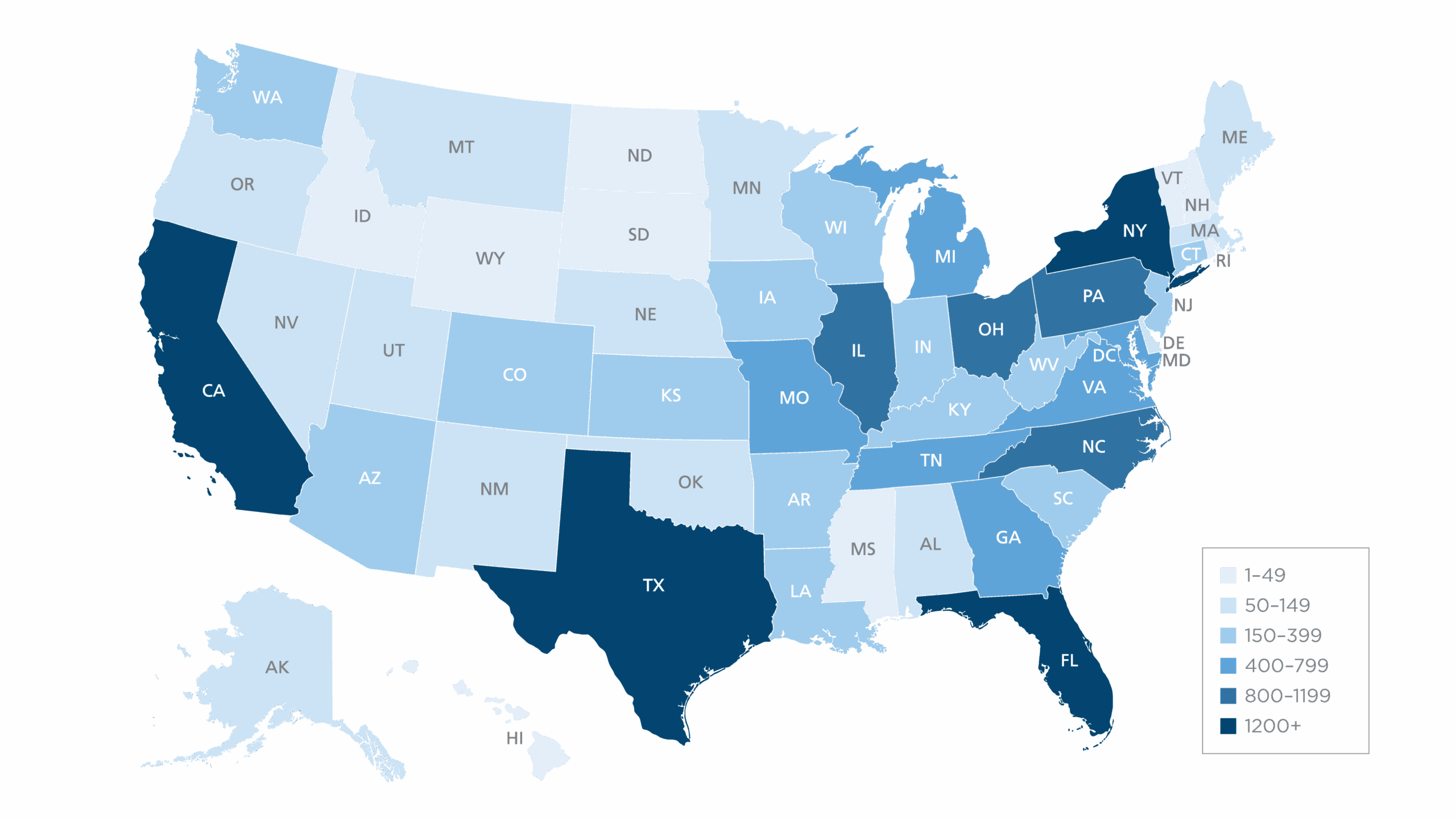
WHEN OTHER VENDORS GIVE UP, VERISMA STEPS IN
Pain Points We Solve:
- Incomplete or failed retrievals
- Provider access issues
- Lack of provider visibility
- Escalated payer frustration
How Verisma Helps:
- Re-attempts failed or missing records
- Resolves complex requests with HIM-trained experts
- Boosts closure rates and lowers administrative strain
- Increases visibility, control, and compliance between providers and payers
STAY AHEAD IN VALUE-BASED CARE
Blog
Preparing for RADV Audits: Key Considerations for Health Plans
Webinar
RADV Webinar Series Part 2: Updates for Payers
In an effort to crack down on fraud, waste and abuse (FWA) in Medicare Advantage (MA) plans, the Centers for Medicare & Medicaid Services (CMS) announced a sweeping initiative in late May 2025. CMS is fast-tracking the completion of outstanding Risk Adjustment Data Validation (RADV) audits—and launching a significantly expanded round of new audits starting September 1, 2025.
Webinar
HEDIS Measure Years 2025 and 2026: Helping Providers and Health Plans Prepare
The Healthcare Effectiveness Data and Information Set (HEDIS®) is the measurement tool used by the nation’s health plans to evaluate their performance in terms of clinical quality and customer service. More than 235 million people are enrolled in plans reporting HEDIS results, making it one of healthcare’s most widely used performance tools.
Webinar
RADV Webinar Series Part 3: Latest and greatest updates.
In an effort to crack down on fraud, waste and abuse (FWA) in Medicare Advantage (MA) plans, the Centers for Medicare & Medicaid Services (CMS) announced a sweeping initiative in late May 2025. CMS is fast-tracking the completion of outstanding Risk Adjustment Data Validation (RADV) audits—and launching a significantly expanded round of new audits starting September 1, 2025.
Let’s build the future of Value-Based Care,
TOGETHER.
